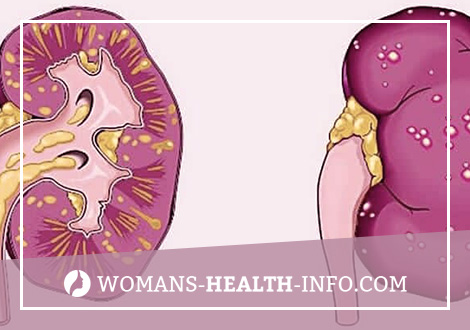
What is Pyelonephritis?
Pyelonephritis is understood as an inflammatory process in which not only the renal pelvis and calyx are involved, but also the renal parenchyma with a predominant lesion of interstitial tissue. In most cases, the disease occurs in women under 40 years old, in some of them during pregnancy. In old age, men get sick more often than women. This is due to urinary stasis due to the development of prostate adenoma. Often pyelonephritis complicates the course of diabetes.
There are primary, or uncomplicated, pyelonephritis and secondary – complicated. Primary pyelonephritis is not preceded by any disturbances on the part of the kidneys and urinary tract; secondary pyelonephritis is based on organic or functional processes in the urinary tract that disrupt the dynamics of urine. Primary pyelonephritis is much less common than secondary.
The causative agents of pyelonephritis are most often Escherichia coli, enterococcus, Proteus, staphylococcus. In most cases, the urine flora is mixed, and in chronic pyelonephritis, mixed flora is much more common than in acute.
During treatment, the urine flora and its sensitivity to antibiotics change. Pyelonephritis is usually preceded and accompanied by bacteriuria. Bacteriuria is absent only with obstruction of the corresponding ureter or the formation of a turned-down abscess in the renal parenchyma.
Pathogenesis during Pyelonephritis
Essential in the occurrence and development of pyelonephritis is a violation of the state of the macroorganism, the weakening of its immunobiological reactivity. A decrease in the body’s resistance to infection as a result of overwork, previous diseases, hypovitaminosis, excessive cooling, circulatory disorders, chronic diseases, etc., as well as massive infection of the body, are very predisposing to pyelonephritis.
Disorders in the outflow of urine followed by urostasis (narrowing and kinks of the ureter, nephrotosis, anomalies of the urinary tract, pressure on the urinary tract from the outside) is one of the main factors predisposing to pyelonephritis.
Pyelonephritis is favored by diabetes mellitus, gout, nephrocalcinosis, potassium deficiency, analgesic abuse, extrarenal foci of inflammation (enteritis, frequent tonsillitis, pneumonia, suppuration), as well as inflammatory processes of the urogenital sphere (prostatitis, cystitis, adnexitis, and adnexitis). .
In the development of pyelonephritis, a major role is played by a violation of the venous and lymphatic outflows from the kidney, which contribute to the fixation of the infection in the latter.
Urokinematography managed to establish significant changes in the ureter urodynamics in the initial stages of pyelonephritis, when there are still no organic changes in the pyelocaliceal system. There are four ways of infection penetrating the kidney, pelvis and its calyxes: a) hematogenous, b) lymphogenous, c) along the ureter wall and d) along its lumen in the presence of vesicoureteral reflux.
Hematogenous pyelonephritis is a secondary focus of infection that has penetrated the kidney from a primary focus, often located in the urinary tract or organs of the reproductive system. If the infection is introduced into the kidney from a focus located away from the kidney and urinary tract, its causative agents are usually gram-positive cocci (in 90% of cases of staphylococcus).
With localization of the infection in the lower urinary tract, microorganisms can penetrate the kidney through the urinary tract. Of particular importance for the spread of infection are the pelvis-renal refluxes. With them, as a result of increased intrapulmonary pressure, microbes enter the venous or lymphatic vessels of the kidneys into the general bloodstream, and then return to the kidneys with a blood stream.
The appearance of acute pyelonephritis in pregnant women is facilitated by the expansion of the upper urinary tract, which occurs due to hormonal changes and compression of the ureters by the pregnant uterus.
Pathological anatomy of pyelonephritis
The initial stage of acute pyelonephritis is characterized by the presence of large edema of paranephral tissue. At this stage, apostematic nephritis or kidney carbuncle may occur. The inflammatory process in the perinephric tissue can be limited to leukocyte infiltration, but can progress and lead to its purulent fusion.
Even with prolonged pyelonephritis in the kidney, areas of purulent inflammation alternate with areas of sclerosis, and between them there may be islands of completely unchanged parenchyma.
Morphologically distinguish four stages of chronic pyelonephritis. In the first stage, the glomeruli are preserved, uniform atrophy of the collecting tubules and lymphocytic infiltration of the interstitial tissue are noted. In the second stage, some glomeruli are hyalinized, there is a pronounced atrophy of the tubules, a decrease in inflammatory infiltration and proliferation of connective tissue. In the third stage, death and hyalinization of many glomeruli are observed, the urinary tubules are lined with a low undifferentiated epithelium and filled with a colloidal mass. In the fourth stage, the cortical substance of the kidney sharply decreases, consisting in such patients mainly of poor connective tissue with nuclei with abundant lymphocytic infiltration.
Pyelonephritis Treatment
Pyelonephritis is usually treated with antibiotics. They are prescribed either empirically (i.e. already tested), or according to the results of sensitivity to antibiotics of a microorganism excreted during urine culture. Of the recommended drugs, antibiotics with a wide spectrum of action are preferred. Usually with uncomplicated pyelonephritis, antibiotics are prescribed orally. The duration of treatment is at least two weeks, although often the symptoms of the disease begin to disappear in the first 3-4 days of treatment.
Antibacterial drugs for the empirical treatment of bacterial infections of the urinary system, such as Biseptol, fluoroquinolones, ciprofloxacin, levofloxacin, are widely known. Other antibacterial drugs for the treatment of pylonephritis are applicable in the case of insensitivity of the detected bacteria to approved drugs or if the patient is allergic to them. After completion of antibiotic treatment, a control urine test is required to determine the effectiveness of therapy. It includes urinalysis for bacteria, protein, and normal white blood cell count.
For hospitalization of the patient, there are the following indications: high body temperature, chills or repeated vomiting, a real threat of dehydration. In such patients, fluid replenishment and antibiotics are prescribed intravenously. You need to know that a pronounced increase in body temperature, chills require close attention. They can be a harbinger of generalization of the infection (bacteria entering the bloodstream and spreading throughout the body).
If the examination reveals a blockage of one of the ureters with a “pebble” that “blocked” the urine from the kidney, then “minor surgery” enters the fray. The troublemaker is removed using a special device inserted through the urethra into the bladder, and then into the ureter.
After the end of antibiotic therapy and the disappearance of symptoms of pyelonephritis, the doctor may prescribe additional studies, which include:
- intravenous urography (the introduction of contrast into the venous system with its excretion by the kidneys and, accordingly, by x-ray contrasting of their pyelocaliceal system);
- ultrasound examination of the urinary system;
- cystoscopy (examination of the bladder through a cystoscope – a special optical device inserted into the lumen of the bladder through the urethra).
How to protect yourself from pyelonephritis, how to move away from yourself the risk of “picking up” this disease? There are very simple and, most importantly, effective methods that we recommend taking into service.
First, wash the bacteria more often. Do not let them settle and breed. To do this, you need to include more fluids in the daily diet. Water among them should be at least half a liter. Water “nutrition” increases the formation of urine and its renewal. Bacteria do not have time to “catch” for you. At the same time, this step is the prevention of urolithiasis, one of the provocateurs of pyelonephritis.
Secondly, constantly drink cranberry or other acidic juices that are rich in vitamin C. It acidifies the urine, which is not good for bacteria. They are slowly growing.
Thirdly, during hygiene in the perineum, women must follow the rule of wiping: from front to back. This reduces the risk of bacteria from the skin and rectum entering the urinary tract.
Fourth, before intimacy, a toilet of the external genitalia is needed. This reduces the risk of bacteria entering the urinary tract during sexual contact.
Fifth, if the fourth is not fulfilled, then after sexual intercourse it is necessary to urinate and in this way remove the bacteria that got into the urinary tract.
Sixthly, for women with frequent dysuric disorders due to urinary tract infections, it is better to take an antibacterial drug (once or twice) after intercourse.
In cases of stagnation of urine due to structural disorders of the urinary system, surgical treatment that restores normal outflow is also a preventive measure aimed at reducing the risk of recurrence of pyelonephritis.
What threatens pyelonephritis to our body? What can one ultimately expect from him? Uncomplicated pyelonephritis rarely leads to severe kidney damage. Unless, of course, patients have concomitant diseases.
But in patients at risk (children, diabetics, patients with structural disorders of the structure of the kidneys and urinary tract, impaired nervous regulation of the functioning of the bladder), chronic pyelonephritis is possible. It, over time, can develop into chronic renal failure (the inability of the kidneys to remove “toxins” from the body). These are the “pies” obtained.
Prevention of Pyelonephritis
Against the backdrop of such a disappointing prospect, the main recommendation for the prevention of chronic pyelonephritis is the treatment of the main diseases that can provoke it. Such diseases are: urolithiasis and prostate adenomas, as well as diseases accompanied by a violation of the outflow of urine from the kidney. Pregnant women, especially those with multiple pregnancy, polyhydramnios, with a large fetus and with a narrow pelvis, need to carry out bacteriological analysis of urine at least 1 time per month and, according to indications, a study of urodynamics. Physical therapy “does not work” with diseases of the urinary system. Only general strengthening medical gymnastics is used, since chronic pyelonephritis is a specific kidney disease. Frequent pain in the lumbar region does not give the opportunity to engage in physical education regularly and with full dedication. And although physiotherapy is a proven and effective means of combating diseases, it, unfortunately, does not give positive results (with pyelonephritis), except for a temporary improvement in general condition.